Abstract
Latest researches in neuroscience and Gut microbiota have uncovered a fascinating connection between our emotions, the hormones in our bodies, and the bacteria living in our guts. This review is an effort to gather scientific explanations on how our feelings can actually affect the composition of gut microbiota through neurohormones.
Introduction
The human gut gives shalter to trillions of colonies of microorganisms, collectively termed the gut microbiota, which executes essential roles in digestion, metabolism, and immune function. Emerging evidence reveals that emotional experiences—such as stress, anxiety, and positive affect—modulate the composition and function of gut microbiota. Central to this modulation is neurohormonal signaling along the gut-brain axis.
The Gut-Brain Axis: Bidirectional Communication
The gut-brain axis is a two directional communication network integrating the central nervous system (CNS), the enteric nervous system (ENS), the hypothalamic-pituitary-adrenal (HPA) axis, and the gut microbiota. Our feelings and thoughts really do affect how our stomach works and even the types of bacteria living inside our gut. This connection happens through various systems in our body – like the nerves, hormones and also the immune system response. So basically, when we’re in a certain mood or overthinking things, it can actually mess with what’s happening in our gut.
- Endocrine signaling: Neurohormones released in response to emotions, including cortisol, norepinephrine, and serotonin, influence the gut environment.
- Immune mechanisms: Stress and emotion-induced immune changes can impact gut permeability and microbial communities
Emotional States and Neurohormonal Signaling Stress and Negative Emotions
Emotional stress triggers activation of the HPA axis, resulting in increased secretion of corticotropin-releasing hormone (CRH), adrenocorticotropic hormone (ACTH), and ultimately cortisol. These stress hormones have widespread effects on gut barrier function, immunity, and microbial homeostasis.
- Acute and chronic stress can induce rapid shifts in gut microbial composition in both mucosal and luminal compartments[5]. Specific studies in animal models show increased gut permeability, inflammation, and overgrowth of pathogenic bacteria under stress conditions.
- Neurohormones such as norepinephrine and cortisol directly modulate bacterial growth and virulence. In vitro, catecholamines can significantly increase certain bacterial populations and enhance their pathogenicity.
Positive Emotions
Positive emotions correlate with distinct gut microbiome profiles. Individuals exhibiting positive affect and emotion regulation have lower abundance of inflammation-associated bacteria and higher levels of beneficial taxa. Specific metabolic pathways related to energy, coenzyme A, and neurotransmitter synthesis also differ with emotional states.
Emotion Regulation
Cognitive strategies that regulate emotion—such as reappraisal or suppression—can alter neurohormonal output, indirectly shaping the gut microbial community.
Neurohormones as Mediators
Neurohormones serve as crucial mediators between emotions and gut microbiota. They are produced both by host tissues (e.g., adrenal glands, enteric neurons) and in some cases by gut microbes themselves.
Important Neurohormones
- Serotonin: Over 90% of the body’s serotonin is synthesized in the gut, with production regulated by both the microbiota and host cells. Changes in serotonin levels affect gut motility and mood.
- Dopamine: Some gut bacteria (e.g., Bacillus, Serratia) produce dopamine, influencing both gut and brain signals.
- GABA, norepinephrine, acetylcholine: Microbes modulate and respond to these neurotransmitters, thereby mediating stress-related effects on gut ecology.
The Impact of Emotional Disorders
Several mental and emotional disorders—including anxiety, depression, and chronic stress—have been linked to gut dysbiosis[10][5]. Shifts in bacterial taxa, decreased diversity, and increased inflammation are often observed in affected individuals. Novel interventions using probiotics and psychobiotics are being explored to restore microbial balance and alleviate emotional symptoms.
Mechanistic Insights
- Barrier Function: Stress and negative emotions compromise intestinal and blood-brain barriers, facilitating bacterial translocation and contributing to systemic inflammation.
- Microbial Metabolism: Emotional states alter microbial metabolism, impacting energy, vitamin, and neurotransmitter synthesis pathways in the gut.
- Immune Interactions: Emotional distress promotes immune activation in the gut, further shaping the microbiota and increasing risk of gastrointestinal pathology.
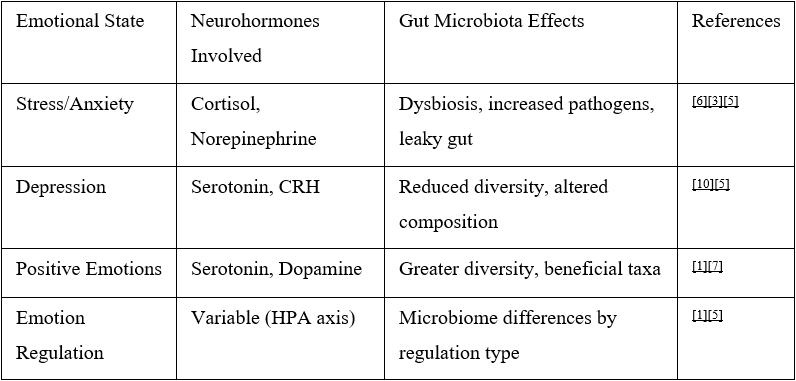
Table: Emotions, Neurohormones, and Gut Microbiota Interactions
Conclusion
Human emotions exert significant effects on gut microbiota through neurohormonal signaling along the gut-brain axis. Stress and negative feelings typically induce dysbiosis, while positive emotional states and effective emotion regulation appear to support a healthier gut microbial landscape. Continued research in this area may hold promise for innovative therapies targeting the microbiome to promote both mental and physical well-being.

Author Name
Professor Dr. Kartikey

